Blood donation plays a vital role in strengthening public health systems across the world. Hospitals, emergency services, and healthcare providers rely heavily on donated blood to save lives and deliver timely treatment. Without a steady supply of blood, even the most advanced medical systems would struggle to function effectively.
This article explains why blood donation is essential for public health and how it supports healthcare infrastructure, emergency care, and patient survival.
1. Ensures Life-Saving Emergency Care
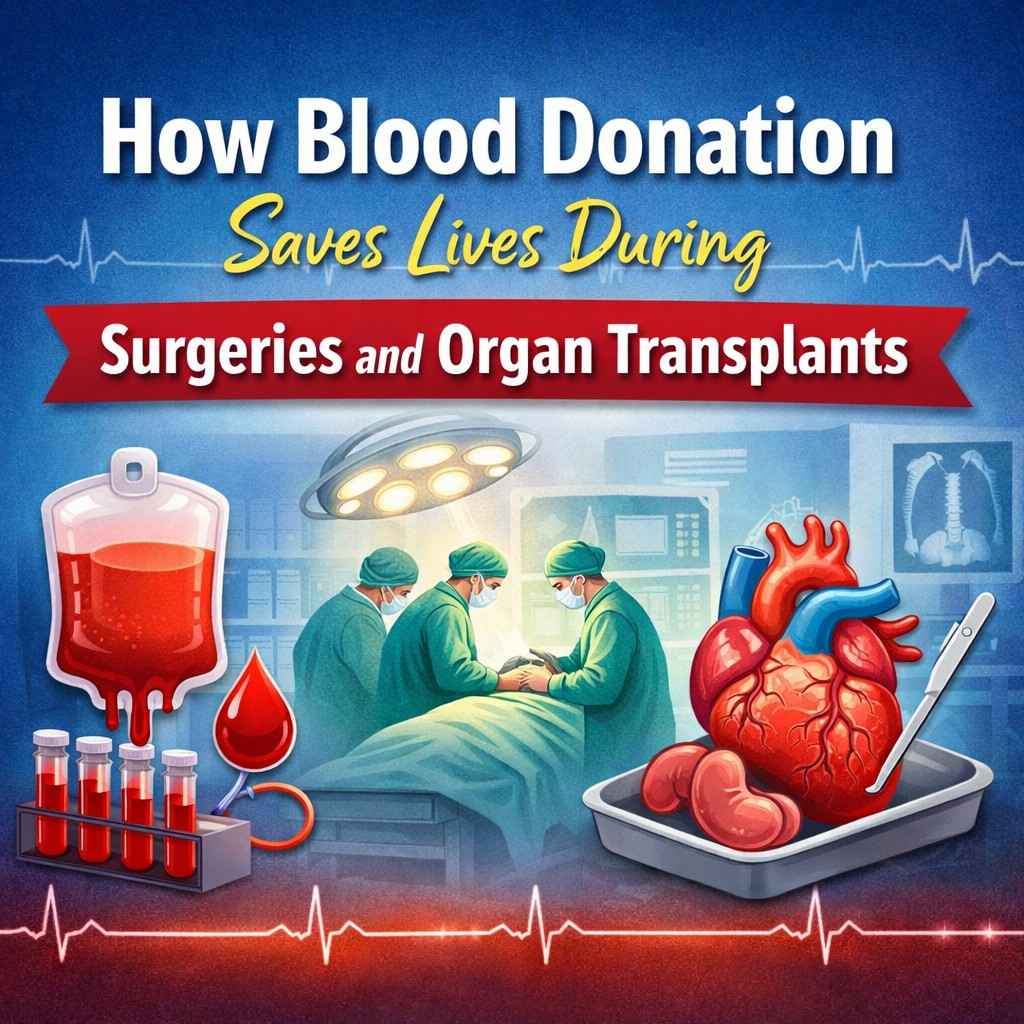
One of the most critical roles of blood donation is supporting emergency medical situations. Road accidents, natural disasters, childbirth complications, and surgeries often require immediate blood transfusions. In such cases, delays in blood availability can mean the difference between life and death.
Public health systems depend on a stable blood supply to respond quickly to emergencies and provide immediate treatment when every second counts.
2. Supports Routine Medical Treatments
Blood is not only needed during emergencies. Many patients depend on regular transfusions for ongoing treatment. This includes people undergoing chemotherapy, individuals with blood disorders like thalassemia, and patients recovering from major surgeries.
Without voluntary blood donors, hospitals would face shortages that could delay essential treatments. A reliable donor base helps public healthcare facilities operate smoothly and maintain quality patient care.
3. Strengthens Healthcare Infrastructure
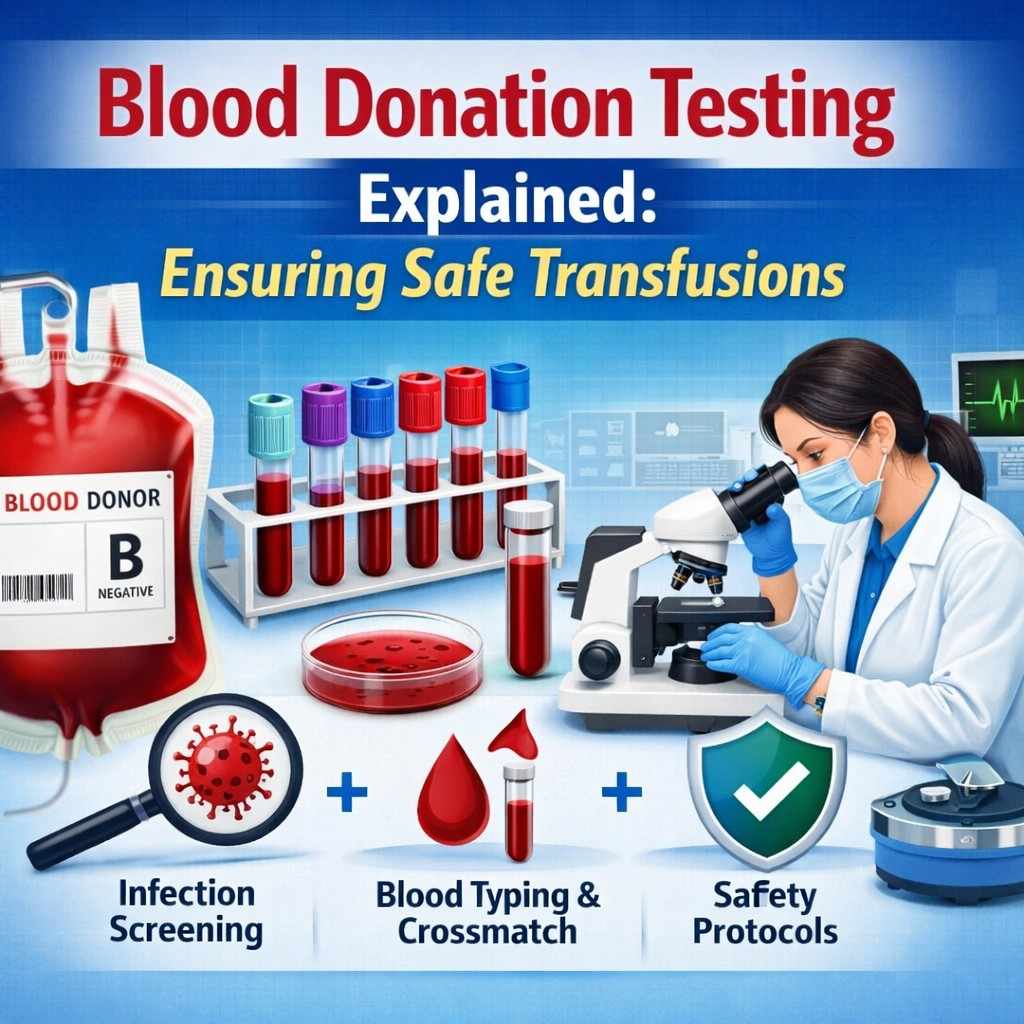
A strong blood donation system improves the overall healthcare infrastructure. Blood banks, storage facilities, and testing laboratories work together to ensure blood safety and availability.
When public participation in blood donation increases, health systems can better plan inventory, reduce wastage, and manage distribution efficiently. This results in improved service delivery and reduced pressure on hospitals.
4. Improves Disaster Preparedness
Natural disasters, pandemics, and large-scale emergencies place enormous pressure on public health systems. During such times, the demand for blood rises sharply.
Regular blood donation helps build reserves that can be used during crises. Prepared blood banks allow healthcare authorities to respond faster and save more lives when unexpected situations occur.
5. Promotes Community Health Awareness
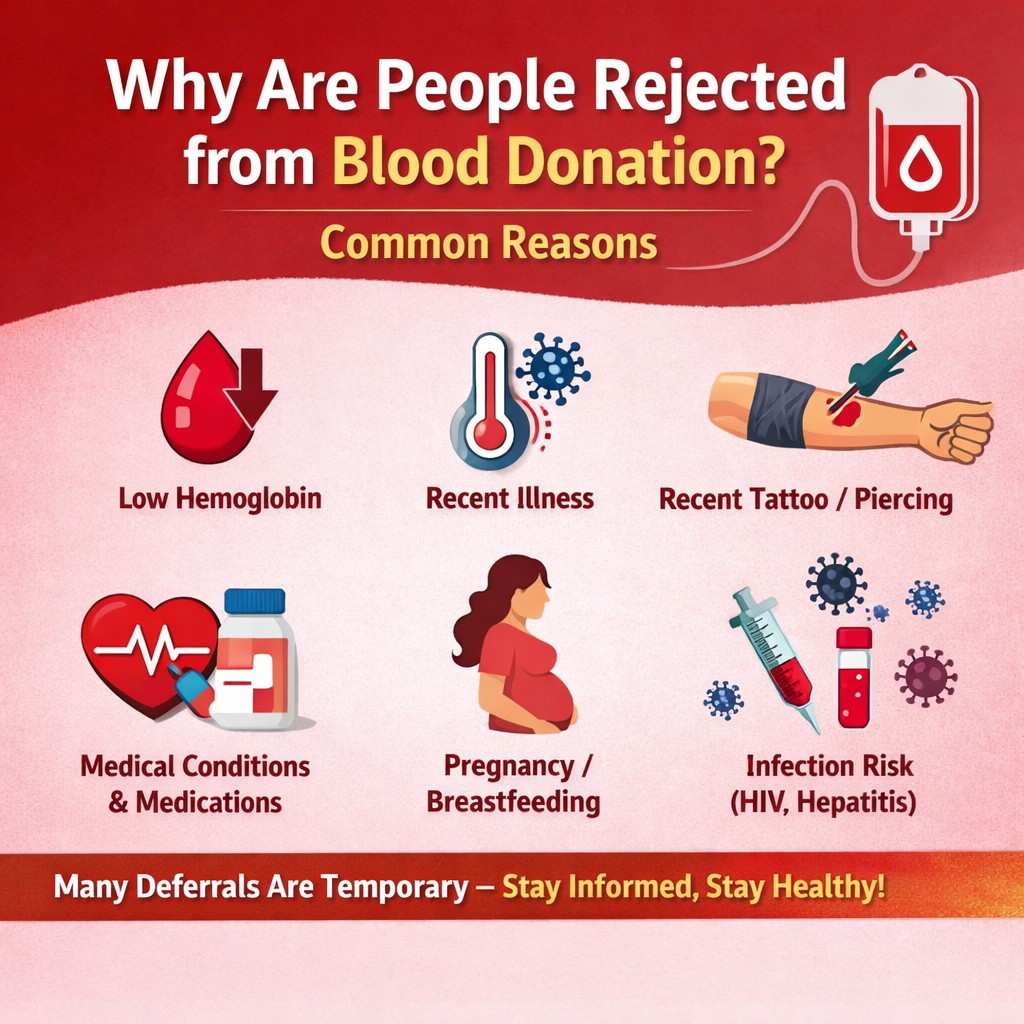
Blood donation campaigns help spread awareness about health, hygiene, and preventive care. Many donation centers conduct basic health screenings such as blood pressure checks, hemoglobin tests, and infectious disease screening.
These programs encourage people to become more health-conscious and contribute to early detection of medical conditions, benefiting both individuals and society.
6. Encourages Voluntary and Ethical Healthcare Practices
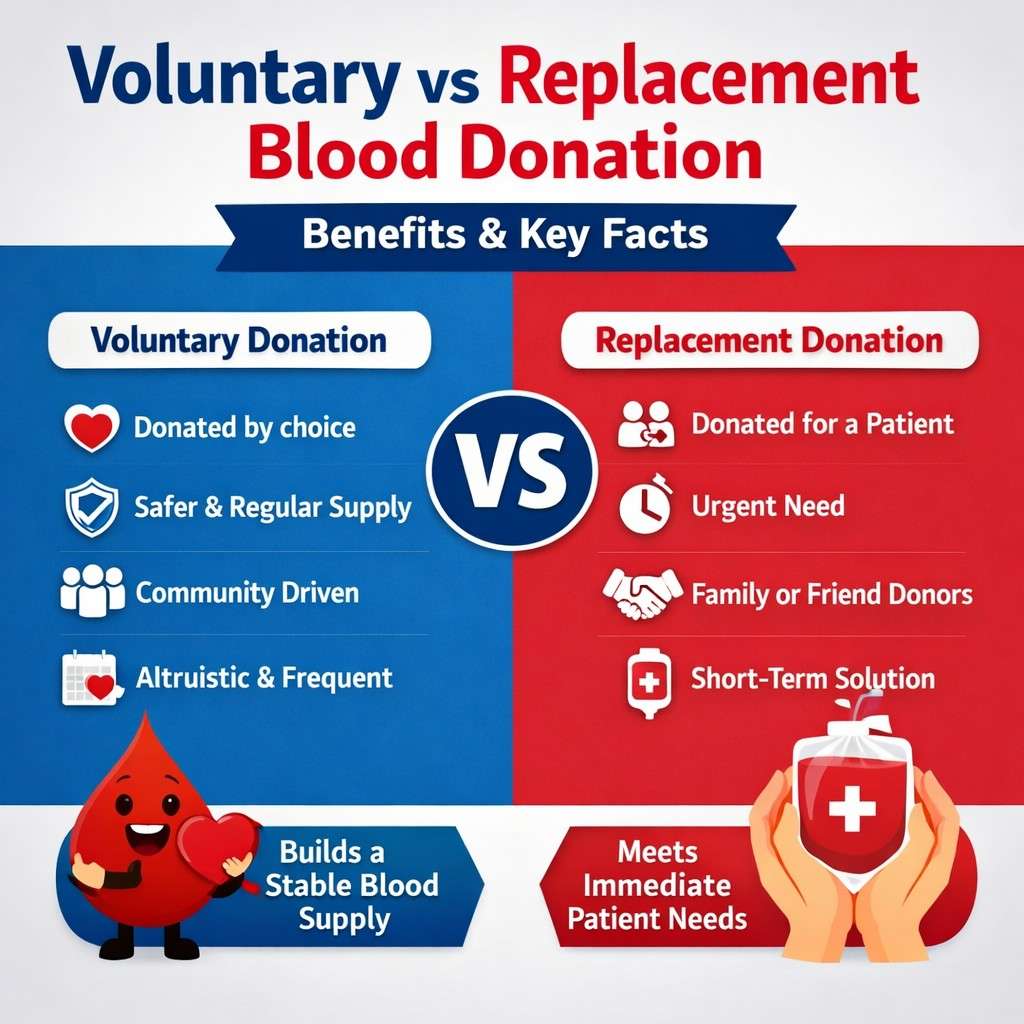
Public health systems rely on voluntary blood donors rather than paid donations. Voluntary donation ensures a safer blood supply and promotes ethical healthcare practices.
When people donate blood without financial motivation, the risk of unsafe donations decreases. This helps maintain high safety standards and protects patients from transfusion-related infections.
7. Reduces Healthcare Inequality
Blood donation supports equal access to healthcare. Government hospitals and public blood banks provide blood to patients regardless of their financial status.
This ensures that life-saving treatment is not limited to those who can afford private healthcare. Blood donation helps create a fair and inclusive healthcare system that serves all sections of society.
8. Builds a Culture of Social Responsibility
Blood donation encourages civic responsibility and compassion. When citizens actively participate, it creates a strong sense of community support.
A culture of regular blood donation strengthens public health systems by turning healthcare into a shared responsibility between governments and citizens.
Conclusion
Blood donation is not just an act of kindness — it is a critical pillar of public health systems. It ensures emergency readiness, supports routine medical care, strengthens healthcare infrastructure, and promotes ethical medical practices.
By donating blood regularly, individuals contribute directly to saving lives and improving the quality of healthcare services. A strong public health system begins with community participation, and blood donation is one of the simplest yet most powerful ways to make a real difference.